Virginia Dermatology & Skin Cancer Center
 Dr. Brian L. Johnson began his medical training at the Uniformed Services University of the Health Sciences in Bethesda, Maryland. His Navy medical career included service aboard the USS Yellowstone, the Kearsarge and the Iwo Jima. He participated in major deployments and field assignments with the Seabees and Special Forces.
Dr. Brian L. Johnson began his medical training at the Uniformed Services University of the Health Sciences in Bethesda, Maryland. His Navy medical career included service aboard the USS Yellowstone, the Kearsarge and the Iwo Jima. He participated in major deployments and field assignments with the Seabees and Special Forces.
He studied dermatology at Johns Hopkins, and completed a Mohs Surgery Fellowship at Northwestern Skin Cancer Institute in Chicago. He’s a Fellow of the American Academy of Dermatology, the American College of Mohs Surgery, and the American Society of Dermatologic Surgery.
Dr. Johnson wanted to really make a difference in his patients’ lives. He soon realized that was dermatology: “I grew up with it,” he says. “My father, Dr. Bernett L. Johnson, was a renowned master dermatologist who subspecialized in dermatopathology, and I knew that there were cases – like melanoma – where I could literally save lives.”
He also realized that dermatology was very diverse: his father’s specialty, dermatopathology, focuses on the study of cutaneous diseases and their causes at the microscopic level. Where Dr. Bernett Johnson enjoyed looking at samples under the microscope, his son preferred the hands-on approach of treating patients in the surgical setting.
During his Mohs fellowship, Dr. Johnson knew he had found a niche. The ground-breaking surgical procedure for treating skin cancer lesions was developed by Frederic Mohs in the late 1930s. “He developed the technique of removing skin cancers and looking at the margins immediately,” Dr. Johnson explains, but relates that the procedure wasn’t adopted by general surgeons at the time because during those years, “skin was considered a non-issue. If you weren’t an internist or a general surgeon, you weren’t considered a real doctor,” he says. Dr. Mohs tried to publish his findings, but surgeons then weren’t comfortable learning skin pathology and laboratory techniques, while dermatologists, who are well versed in dermatopathology, and who routinely treated skin cancers, embraced the procedure.
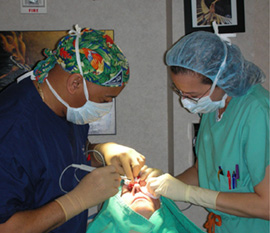 “Dermatologists picked up the technique and ran with it,” Dr. Johnson says, “and over the years, we’ve refined it to the point where we can use local anesthesia, remove the cancers and evaluate the margins under the microscope while the patient is waiting. It’s easier on the patient in many ways – notably, it completely eliminates the anxiety of having to wait days or even weeks for a biopsy report, or to have the wound repaired.”
“Dermatologists picked up the technique and ran with it,” Dr. Johnson says, “and over the years, we’ve refined it to the point where we can use local anesthesia, remove the cancers and evaluate the margins under the microscope while the patient is waiting. It’s easier on the patient in many ways – notably, it completely eliminates the anxiety of having to wait days or even weeks for a biopsy report, or to have the wound repaired.”
Dr. Johnson can perform as many as 10-15 surgeries in a typical day. When his patients arrive for their Mohs surgery, they expect to stay a while, because the entire process can take several hours. Some are there all day – which leads to one of the most fascinating non-medical aspects of Dr. Johnson’s practice: after their initial incision, patients are bandaged and sent to Dr. Johnson’s waiting room. While they wait for their tissue to be processed and read – a process that can take up to 90 minutes – they become part of a small fraternity. “Some patients are self-conscious about going into the waiting room with bandages on their face,” Dr. Johnson says, but adds their embarrassment is short-lived, because in his waiting room, everyone has bandages – on their ears, noses, cheeks: anywhere on their face or neck. “They don’t even think about it, because everybody is bandaged,” he says. “They may start out watching TV or reading – but they always wind up talking to each other. They trade stories about how they got their cancers, and conversation grows from there. It lessens the anxiety.”
Some of his patients have been coming to him for years, and he sees them calming down some of the newer patients. “It’s incredible,” he says. “The waiting room evolves into a big support group.”
“Mohs surgeons are really three doctors in one,” Dr. Johnson says. “We’re oncologists, cutting out cancers. We’re pathologists, reading the slides to make sure all the margins are clear. And we’re reconstructive surgeons. We perform all three functions.”
From the patients’ standpoint, that efficiency means everything is dealt with on the same day, so they’re spared the ordeal of waiting for pathology and follow-up appointments. The cost savings can be substantial, but many think the convenience and lessened anxiety are even more important.
Dr. Johnson’s passion for surgery and providing a family-friendly environment was an integral part of his motivation to build a 16,000 square foot, state-of-the art medical facility in Norfolk. The building was designed to provide patients with unparalleled convenience for general, surgical, and cosmetic dermatology services under one roof. The building is equipped with the latest technology to treat the diseases of the skin, hair, and nails. In addition, the facility offers an exclusive cosmetic dermatological suite with the most innovative technology for aesthetic and body contouring procedures.
Dr. Johnson says, “We found it necessary to become a larger organization to help counteract the many negative changes in healthcare that inhibit a provider’s ability to adequately care for and treat patients – notably, insurance companie’s control of what procedures we can perform or what medications we can prescribe and pharmaceutical companie’s exorbitant pricing of prescriptions. “Many of my patients can’t afford to get the medications we feel are best to treat their condition,” he says. “I was absolutely horrified when a patient told me that she spent $800 out-of-pocket for a small tube of ointment because I recommended it. Things won’t change until physicians come together as a group and demand a change. The system does not run without us.”
Dr. Johnson’s top priority remains to promote outstanding quality healthcare through education, and providing patients with the highest level of personalized care in a family-friendly environment.

